My husband and I were newlyweds when I received a bizarre diagnosis regarding my placenta. We were still trying to wrap our heads around the fact that I was pregnant in the first place. Spring chickens we were not: Charlie was 47 and I was 40 when I became pregnant with twins. It was a shock to both of us, to our families including my college-age stepsons, and even to my OB, who immediately advised me to refrain from exercise and “physical intimacy.” He also sent me to a specialist for a risky procedure called chorionic villus sampling (CVS), a test that would determine whether chromosomal or genetic disorders were present in my fetuses. At the time, I was ten weeks pregnant.
The specialist who conducted my CVS procedure was a soft-spoken man with wiry dark hair. “Huh,” he said, while reviewing the monitor where two black dots danced blurrily across the screen. He rubbed his forehead and frowned. “One of your babies is large for its gestational age and the other is quite small. It appears as if you have twin to twin transfusion syndrome [TTTS].”
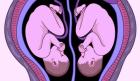
Because I was silently congratulating myself for producing something large (all my life I’d been critiqued for my non-athletic frame, my toothpick-like arms and legs), I nearly missed the doctor’s concern. Or maybe I wanted to. I don’t like to be bombarded with details, especially when bad news is involved. I wasn’t prepared to hear about a random syndrome that affects identical twins, a disease of the placenta that causes one twin to inadvertently “steal” blood (which carries oxygen and vital nutrients) from the other. I wanted to believe I was capable of growing two healthy babies, even at my advanced maternal age.
But the doctor didn’t let me off the hook. “We need to keep an eye on you. This can become quite serious.” His expression made me pause. “You’ll need to be monitored frequently,” he said. “Your pregnancy was already considered high-risk, and this ups the ante.”
The smaller twin, the one dubbed the TTTS “donor,” was identified as Baby A by the doctors. Baby B, the larger “recipient” twin, was at an advantage when it came to nourishment provided by my placenta. His umbilical cord was attached more centrally; Baby A’s was hanging on near the end. I didn’t learn about this for several weeks, though. In the meantime, I was barraged with questions from friends and relatives.
“Aren’t you mad at Baby B?” asked one horrified aunt. “Wonder if he’ll always be like that – taking what isn’t his.”
“Of course not,” I replied. “It’s not his fault.”
“It’s the craziest thing I’ve ever heard of,” said a friend. “Are you sure the doctor knows what he’s talking about?”
What I read about TTTS kept me up at night. What if I was upset with Baby B, even subconsciously? Would it impact the way I treated him? Would Baby A always be the smaller, “weaker” twin? If so, would I coddle him? Automatically place blame on his brother when they fought?
The doctors seemed most concerned about Baby A: His growth was slow, his amniotic fluid low. At each bi-weekly ultrasound appointment -- nerve-wracking sessions that I dreaded -- Baby A was examined every which way. The specialist’s mouth usually formed a tight thin line as data was analyzed.
Worst of all was a question that repeatedly turned around in my head: What if neither baby made it? According to TTTS statistics, both twins are at risk for early termination. The one receiving too much blood can die from cardiac arrest; the one receiving too little can expire from inadequate growth.
My fears were nearly realized when I went into pre-term labor at 23 weeks. Even though I knew something was wrong and that I needed to get to a hospital at once, I didn’t understand the gravity of the situation. Shortly after admittance, a nurse yelled at me when I got up from my stretcher to use the bathroom. “You are in labor!” she screamed. “You cannot get up!”
She couldn’t have been more prophetic. For the following four weeks, I was on hospital bed rest. A cerclage procedure was conducted to close my cervix, anti-contraction medicine was pumped into my veins, and steroid shots were administered – intended to promote my babies’ lung development. I was rarely allowed to shower or use the commode, and I was instructed to lie on my left side, at all times, even while eating, to help reduce pressure on my cervix.
“Your number one priority is to stay calm,” said my OB. “We want those babies to remain inside you as long as possible.” I was uncomfortable, frightened, and embarrassed about my loss of hygiene, but it was a small price to pay. I would do whatever it took to create healthy outcomes for my children.
One night, about a week into my hospital stay, a prenatal specialist appeared at my bedside with an ultrasound machine. Baby A didn’t look good, she said. I should prepare for his loss; it was only a matter of time.
Later that evening, my OB entered the room. “I heard the news,” he said, folding himself into a chair against the wall. “But if all goes well, you’ll go home with one healthy baby.” His blue-gray eyes were tender and he spread the palms of his thick hands upward, as if in apology.
“No,” I said in a clear, firm voice. “Baby A has made it this far and he’s going to keep making it. I’m not giving up.” The finger I’d been pointing in protest toward my doctor’s direction hadn’t even trembled. For the first time in my life, I found purpose, a steel will. No one was going to write off my cubs.
Cards, flower bouquets, and gifts showered my room. I wrote in a journal several times a day and talked aloud to my unborn children. “We’re a team,” I told them. “Take good care of my family,” my husband said as he departed from nightly visits. His tall frame filled the doorway but his shoulders had begun to stoop.
Before my hospitality, prematurity had barely entered my thoughts. I’d been too focused on TTTS, too absorbed with wishing the doctor had made a mistake. Or that my smaller twin would magically catch up.
As a patient in the maternal-fetal care unit, however, prematurity became a consuming concern. It was decided that my twins would be delivered by caesarean section at 28 weeks. Survival odds for babies born at that gestational age were quite good, said the doctors. Due to the progression of TTTS, my womb was becoming less safe. I was told that neonatologists would soon meet with me to discuss health risks associated with prematurity, including under-developed central nervous systems, brains, and other internal organs.
“Will their heads really be the size of lemons?” I asked, nervously, when I phoned my sister after digesting a book she’d sent me about what to expect. She, too, had given birth prematurely. Her son was now a healthy-nine-year-old and my sister assured me that my children would be healthy, too. She had no way of knowing that, but it’s what I clung to.
A few days later, on a Thursday, contractions wracked my body with alarming frequency and severity. I rang for the nurse and shortly after, my OB prepped me for an emergency C-section. Baby A’s amniotic fluid was dangerously low. I was four days shy of 28 weeks. While we waited for my husband to join us in the delivery room (he was forty miles away, driving through a downpour), my nerves stretched and expanded, like rubber bands near their breaking point.
“What kind of music do you want to hear?” my hip Los Angeles doctor asked. “The Beatles? Aerosmith? Please don’t say jazz or classical,” he groaned, jokingly, and grabbed his stomach.
For the first time in my life I didn’t want to hear music. “Please don’t play anything,” I tried to say, but my teeth were chattering uncontrollably and my tongue was thick and dry, unable to form words.
“Hey babe, I’m here,” a muffled voice finally said. It took me a moment to register my husband’s beautiful green eyes, the kindest eyes I’ve ever known, floating above a medical face mask. He clasped my cold hand in his.
Baby A (Jack) arrived soon after, weighing one pound, twelve ounces. Baby B (Sam) appeared four minutes later and weighed two pounds, thirteen ounces. My husband sucked in his breath. Sam was the color of beets, he told me. An overload of blood had taxed his system.
Activity filled the room. Sam was taken away to intensive care, in urgent need of assisted lung ventilation. Wait! I tried to shout. I wanted to see my son first, before he left, but I couldn’t extend my arms to reach out; they were unmovable. And my voice was faint.
I did however, get to see Jack shortly after his birth. “Here’s one of your miracles,” a nurse had said. She held him close to me, near my face. He was wrapped tightly like a burrito in a blue and white blanket, his frail body covered for warmth.
“Hello, sweetie,” I whispered. Jack’s left eyelid fluttered and then a tiny blue eye opened and stared back at me. It was just a slit, a sliver of blue on a head the size of a lemon, but there it was. There he was. I didn’t blink. I didn’t breathe. I just lay on the delivery table, taking it all in.