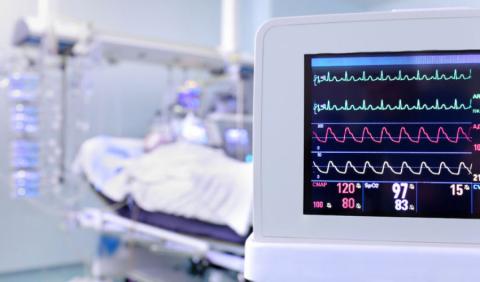
In a recent interview with Cosmopolitan Magazine, actress Kate Hudson stated that the laziest thing she had ever done was “have a C-section.” Indeed, her opinion that opting for a Caesarean section over a vaginal birth is taking the easy way out is one that is shared by many women and has been for some time, and it led me to go against my gut when deciding how to deliver my daughter with disastrous results.
It was June 30, 2002 and I was four days past my due date. Twelve years after giving birth to my son and after four long years of unexplained infertility, my daughter Kathleen (aka Katie) was about to make her appearance. Because my son had been born in via Caesarean section after thirty-three hours of labor, when I got pregnant with my daughter I was given the option of having another Caesarean section or attempting a VBAC (Vaginal Birth after Caesarean). My doctor and the other obstetricians in the practice strongly urged me to choose the VBAC, since it was safer for myself and the baby, I’d have a shorter recovery time, and the risk of uterine rupture was less than one-half of one percent. “Those are pretty good odds!” they told me, again and again. At one point I said I actually was leaning more towards another Caesarean section and my doctor was appalled, asking me why on earth I would want to do that.
My best friend was, excitingly, also pregnant, due four months before I was. When her son was born safely via VBAC and she shared how much easier her post-partum recovery was, it seemed to be the best choice.
The night of June 30th I woke up with abdominal pain. Since I’d never really gone into labor with my son I didn’t know what it felt like so off we went to the hospital. I was put into a gown, had a fetal monitor strapped to my belly, and was promptly told I was not in labor.
“I don’t know,” I told the nurse. “This pain is pretty bad. I’m also a few days past my due date. I think I might want to have a C-section after all.”
The nurse rolled her eyes at me and said “Yeah, I see a lot of people who want to take the easy way out. The doctor said to send you back home. Don’t come back until the pain is so bad that you can’t talk when you’re having one.” I left feeling embarrassed and ashamed.
I spent the next twenty-four hours trying to relax. Katie wasn’t moving much, but I knew that was common because the baby had very little room to move around. Once again, after midnight, the pain became very sharp but not debilitating. Still, I could not shake the feeling that something was wrong so we returned to the hospital. This time when they strapped the fetal monitor belt to my abdomen there was no reassuring “thump-thump-thump” from her heartbeat. The nurse went to get the intern to do a sonogram, all the while telling me not to panic, but I had a cold knot of fear in my stomach.
The intern came quickly and was also unable to find a heartbeat, but she told me cheerfully “Don’t worry. I don’t do these things very well. The doctor is on her way in and she’s much more skilled at finding the heartbeat.” I wish to this day that she had not given me that false hope that everything might still be okay.
The doctor breezed in about half an hour later, smiling, saying “I’m so sorry, these things just happen sometime.” I thought she meant the intern not being able to find a heartbeat, but she meant that my daughter had passed away in utero. I thought then I would get my C-section, but the doctor insisted that I still try to deliver her naturally and assured me I would get a lot of medication for pain “…now that the baby is not a consideration.”
They gave me medicine to induce labor and put a needle in my spine to block the pain but I was still in agony. The nurses treated me like I was being unreasonably demanding when I cried that the pain was unbearable. The doctor came in, again all smiles, around 10:00 pm and said that if I did not deliver by the morning they would do a C-section. At 1:00 am, however, I felt that I would lose my mind from the pain. Things just did not feel right. My husband went to the nurse’s station and demanded a surgeon be called. I will never forget the look of shock and horror when the surgeon walked into the room and saw me. I was wheeled to the OR immediately and had to be put under because the spinal block was not preventing me from feeling the surgery. Later I would find out that my uterus and bladder had ruptured and Katie was in my abdominal cavity. A doctor I saw a few months later looked at my medical records from that night and said “My GOD – how did you not die?” My simple answer was “I didn’t know I was supposed to.”
Afterwards I was wheeled to my room and the nurse promised my daughter would be brought to me. I was nervous about what she was going to look like, but she was just like any other precious newborn. Her skin looked flushed and her lips had a purplish hue, but otherwise she was beautiful. The very kind nurses took pictures and saved a lock of her hair for me, but when the doctor handed her to me she said bluntly “I have patients to see in my office at 8:30 so I have to be out of here by 8:00 am.” It was 7:50 at that point, so I only spent ten minutes with my precious baby. I wonder now how I didn’t tell the doctor too damn bad, I’d take as much time as I needed, but I guess I was so heavily medicated I wasn’t thinking straight.
The Internet was not as vast as it is now so information was not as readily accessible, but I did find a fantastic support group of people who had also suffered uterine rupture during a VBAC. Through the resources provided to me, I discovered that I should never have been a candidate for a VBAC due to some issues I’d had during my son’s birth 12 years earlier. My husband and I consulted an attorney who reviewed my records from that night and said that most likely my uterus had begun to rupture the first night I went to the hospital and was sent back home, and if they had kept me there on a fetal monitor Katie’s life may have been saved. We were also told that we had no case because I had consented to a VBAC and unfortunately, a stillborn baby had no value in the eyes of the law.
It’s amazing how much the death of a child causes people to tiptoe around you while other people seemed to feel that because the baby never took a breath it wasn’t like losing a child at all. When a store clerk I’d seen frequently asked me where the baby was and I said she’d died, the woman shrugged her shoulder and said “Eh. Have another one.” Like my garage sale had been rained out. The Human Resources department at my job called and said “We know you’d planned to take twelve weeks of maternity leave, but since you don’t have a baby do you think you’ll come back earlier?”
I find comfort in the fact that my experience has been used as a teaching case in some maternity wards, and believe it or not I am not opposed to VBACs. I just urge women considering one to utilize an obstetrician who is experienced with the VBAC process, and to absolutely not go past their due date, because that is when most uterine ruptures occur.