My husband walked a little ahead of us on the trail. We were hiking in Pisgah National Forest for the day, on the hunt for waterfalls. My son was on my back in a carrier, pointing out the birds that flew overhead and the stream visible over the ledge. The crunch of rocks and dirt underfoot was muted by the full trees and undergrowth along the sides of the worn path. I stopped to take a sip of water and realized that my thighs were beginning to tighten and burn.
Man, I’m out of shape, I thought, but then I smiled. This felt good. Really good.
We hadn’t been on vacation in four years, and this was the first trip we had taken with our son, who had just turned three. Instead of heading to our favorite island in the Outer Banks, we opted for the mountains in Western North Carolina. My husband and I agreed that a week of hiking and exploring the small towns around Asheville sounded much better than sitting in beach chairs for a week. After a sedentary semester of grading papers and lesson planning, I needed to get out and move.
Some people might call it a premonition — I don’t know what to call it. What I do know is that day on the trail, I had a feeling. I needed to appreciate being able to hike with my family. I felt it in my bones. I couldn’t take for granted my ability to be active, to get outside and walk, run, jump. Some people can’t do this, I thought. Some people will never be able to do this. I felt grateful for the burning in my legs and the sweat on my forehead. I vowed to be more active simply because I could.
Maybe it’s just human tendency to try and link experiences together that are purely coincidental. Looking back now, though, I see a common thread woven through that hike and two other events.
A few months before our trip, I read a blog post by a writer who made a New Year’s resolution to take 10,000 steps per day. The writer reflected on her appreciation for her body’s capabilities. Movement, she argued, is an ability we should not take for granted. At the time, I appreciated the sentiment. But I just smiled, closed the post, and began reading something else. It didn’t have the significance for me then that it has for me now.
A few weeks after reading the blog post, I started watching the film Cake starring Jennifer Aniston. The film is about a woman who deals with chronic pain. As I watched the events play out on screen, I had a visceral reaction. I could not bear to watch her struggle just to stand, just to sit, just to make it through the day. I got through the first twenty minutes of the movie — then I had to turn it off.
I thought about that film often in the months leading up to our trip. I couldn’t shake it.
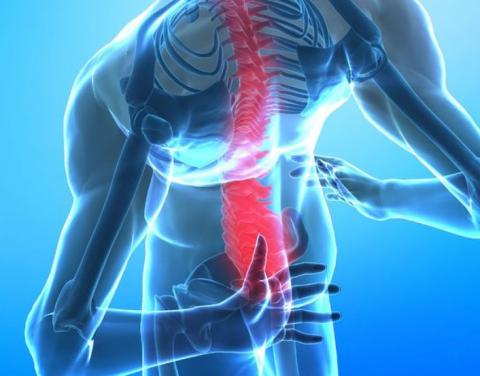
Three weeks after the hike in Pisgah Forest and our return home from North Carolina, I woke up in the middle of the night. My back was aching.
I rolled over onto my stomach. A stabbing pain shot down my lower back and into my left leg. Tears stung my eyes and I froze. I couldn’t move — the pain was too intense — but I needed to move, to escape. Maybe if I get up and walk, I thought, that will help. I slowly rolled back over onto my right side and took a deep breath. Using my arms, I forced myself into a sitting position. The searing heat shot down my leg again; now the tears were flowing freely.
“Babe?” I whimpered. Please wake up, please wake up. My husband’s deep breathing continued. “Austin?” I pleaded, a little louder this time. “I need help.”
He rolled over. “What’s wrong?” he murmured, his voice thick with sleep.
“I… I can’t move. It hurts.”
That night was the beginning of three months of intense pain. The next morning, my husband had to pull me out of bed. I couldn’t stand to get out by myself. I cried through my shower. I regretted getting in the minute the water hit me. It hurt. It hurt to raise my arms, to turn around, to pick up the soap, to tip my head back and rinse the shampoo out of my hair, to move my foot forward so I could lean against the shower wall. Everything hurt.
You don’t appreciate what it feels like to move, and I mean really move, until you can’t without being in pain.
The day before I woke up in pain, I had seen my chiropractor for the first time in months. Sitting at my desk at work had been uncomfortable, and I wanted to prevent the discomfort from getting worse. I had been seeing different chiropractors — depending on where I lived — for lower back pain for sixteen years, with the last fourteen being mostly preventative care. After a few adjustments, any discomfort usually faded. This time was different. I had never felt pain this intense, and I hesitated to return to the same practitioner.
After my shower, I made an appointment with a new chiropractor. He took some x-rays, which did not reveal anything obviously wrong. Based on my symptoms, he told me it was sciatica. He explained that sciatica generally occurs when there is pressure on the sciatic nerve, which causes pain to radiate down one or both legs. Usually there is an inciting incident, like a car accident or a bad fall. It was unusual to just wake up in that much pain.
After a month of gentle adjustments three times a week and daily doses of Aleve, my chiropractor ordered an MRI. Lying in the tube on the morning of my scan, I closed my eyes and hoped that the images revealed the answers — that I would finally know the cause of my pain. The MRI showed a bulging disc, which my chiropractor said was most likely the reason for the sciatica.
I got a steroid shot and then a second steroid shot. I tried wearing a brace, going to an acupuncturist, experimenting with different stretches, juicing with celery and ginger, anything to make the pain go away.
Although the pain did ease up, after a while it seemed to stagnate when it should have improved. As time went on, I began to think, “What if it never goes away? What if this is it?”
The thought terrified me. I admitted this to my husband one night, my voice shaking. Saying it out loud might make it true.
I thought of the sciatica group that I had joined on Facebook. Some of the people in that group had suffered from chronic pain for years. I sought out this group for help, but I could barely read the posts. Some people described countless surgeries resulting in little relief; others reflected on their feelings of helplessness and inability to connect with their families and friends because of the pain. Some of the posts were inspiring — they described people recovering, finally able to live without constant discomfort.
But the inspirational stories weren’t reassuring. The fear of living with permanent pain, of missing out on so much with my husband and my son, was too much. My husband reassured me I would get better — that the pain was temporary. I nodded, but the feeling of dread remained.
After doing research, I discovered that although it is rare, uterine fibroids — which run in my family — can cause severe sciatica. I already had major surgery in my twenties to have nineteen fibroids removed. Two years after my son was born, they returned with a vengeance. They were uncomfortable, but I was used to living with them. My chiropractor was doubtful that fibroids were the cause of my sciatica. But when I saw my OBGYN, I learned that if the fibroids are on the back side of the uterus, they can press on the sciatic nerve. The placement of my fibroids was not conclusive in an ultrasound, but my doctor felt confident that they were causing — or at least exacerbating — the sciatica.
I felt relieved to have an answer — although it was not conclusive — and moved ahead with surgery to have the fibroids removed. My doctor was only able to remove about half of them. The back pain eased, but it was still there. My left leg and foot still regularly went numb. While I was thankful to be in less pain, I was frustrated that I still didn’t have definite answers and that the source of the pain had not been identified conclusively.
Two months ago, I sat down in front of a new OBGYN in the city where my husband and I moved our family at the beginning of the new year. She listened intently as I described my various scans and surgeries: abdominal myomectomy at twenty-six, cesarean section at twenty-nine, laparoscopic myomectomy at thirty-two, x-rays in June, MRI in July, ultrasound in November. I handed her photocopies, discs, and reports. I fought the anxiety rising through my chest and into my throat as I tried to explain each issue clearly.
The doctor typed on her computer and asked questions for clarification as she completed her notes. Then she laid out a plan. It wasn’t normal, she said, for me to still be in pain each day and feel the numbness in my leg and foot. She would refer me to a neurologist and schedule a pelvic MRI for the fibroids and a lumbar MRI for the back pain. While she wasn’t ruling out the possibility of the fibroids causing pain, she did not want to overlook an underlying issue. I took a deep breath, daunted by more scans and tests, but also relieved to have a plan.
Nine months after the first MRI, I went into a tube for a second time. On the phone with my doctor five days after the MRI, she explained the results. The pelvic scan confirmed that I had numerous fibroids, but the fibroids were not causing my back pain.
“They’re not?” I asked in disbelief. This was the first conclusive statement I had gotten about the pain. I had not been anticipating the relief I would feel or the fear of what could be causing the pain.
“They’re not,” she confirmed. “The fibroids are not near the area where you are experiencing pain.”
The lumbar scan, she went on to explain, showed significant narrowing of the spinal canal on the left side and moderate narrowing of the spinal canal on the right side. She called it spinal stenosis and said that my symptoms could be explained with this diagnosis. She would refer me to a specialist, who could talk to me about treatment options and help me find relief.
That night, after speaking with my husband about the results, I cried. I was afraid. I was anxious. But more than anything, I was relieved. I finally had some answers.
Today, I am waiting to see the specialist. While I do not yet know what will happen, I am hopeful about the future and thankful the pain is manageable.
I can move. I can sit on the floor to play with my son, I can stand in the kitchen to make dinner, I can go for walks with my family in the evenings, I can sit at my desk to work, and I can make it through an entire film at the movie theater. I even went for a short hike a few weeks ago on the same trail in Pisgah Forest where I stopped, months ago, and vowed to myself to get out and move.
I am aware of my body in a way that I never was before. The ability to move freely without pain — to reach up and hug my husband, bend down to smooth back my son’s hair, turn when somebody calls my name — is one I will not take for granted. I will continue to move.