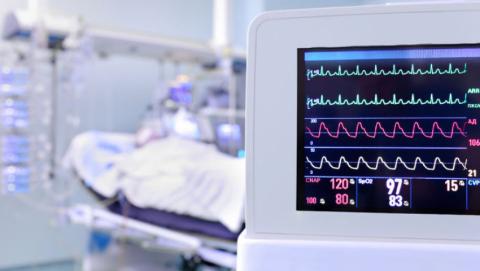
A team of white-coated doctors looking rather grave, stood ranged around my bed in the Intensive Care Unit (ICU) of a Hospital in Pune. I had been hospitalized for yet another attack of pneumonia on 3 September 2018.
The cardiologist, Dr. G, had tried every known treatment on me. Higher, more frequent doses of diuretics to get my kidneys functioning. Vymada and Eptus to make my heart pump more blood into my body, but nothing was working.
The veins on my hands were swollen from milrinone being intravenously infused into me day and night. In vain, the nurses shifted the needle from the left hand to the right but I could get no respite from pain.
I had stopped sleeping at night and was restless like an injured animal. I kept moaning, unable to move my hands numb with the non-stop infusion. I had reached the last stage of heart failure, a fatal malady that I was unexpectedly diagnosed with in 2012.
Dr. G, her brow wrinkled with anxiety, frankly conveyed the news to my sisters that I would not survive. They stood listening to her, their faces pinched, mouths dry.
“Can nothing be done to save her?” They asked.
“A heart transplantation is the only known life-saving intervention. We could invite a renowned heart transplant surgeon from Chennai to review her.” My sisters readily agreed.
Two days later, a dignified-looking, elderly surgeon walked into the ICU to review my condition. I was 69. My age compounded the complexity of my condition. He glanced at my reports, spoke with Dr. G and then said he could not comment until I had cleared a pre-evaluation investigation. He highlighted the risks of the surgery and the possible side effects post-surgery. My family and I decided to go forward.
His cardiac team flew in from Chennai and airlifted me to their hospital for the evaluation, which I fortunately cleared. After a tense ten day wait, a matching donor heart was located. I was transplanted on 4th October 2018 in a 5-hour high-risk operation.
After the miracle surgery, I was fully cured and released from a nightmarish existence.
But my strange story actually began the day my mammogram tested positive. That unforgettable day, my room, my siblings, my mother, all things familiar, suddenly turned unfamiliar. I was 58, fit and had been an established Professor of English, renowned researcher, author, and widely-travelled corporate coach. But on 11 October 2007, clutching the report, I tottered to steady myself against the hospital wall.
“Come”, said my sister holding my hand, Let’s go and meet Dr. S.” Dr. S was a well-known oncologist.
Radical mastectomy and a biopsy confirmed Breast Cancer Stage III. “You’re lucky,” Dr. S said, “to be estrogen receptor-positive but HER2-negative.’”
“What’s that?”
“It’s a condition which gives the patient a better chance of survival.”
The surgery was successful. I was discharged two days later and sent home to recover, which I did quickly. I visited the hospital every other day to get the bandage changed. Soon the drains were removed as blood and other waste secretions cleared up. Everything seemed to be going well.
Three weeks down, Dr. T the medical oncologist prescribed chemotherapy. Epirubian was one of the drugs. I reacted violently within hours of the first cycle and was taken to the hospital, retching.
"What happened?” a nurse asked.
“I can’t stop vomiting.”
I needed medical attention and was hospitalized. As Dr. T walked in briskly to see me, she said in a loud, standoffish voice, “One chemo and off you go!” I was jolted. Dr. T should have investigated but did not.
The smell of chemo medicines in Day Care nauseated. Infants to old people lay on white powder-coated beds receiving chemo. Small children whimpered non-stop. Clouds of misery ballooned. Dr. T never entered Day Care except during an emergency. She never came to pat patients. We always watched her receding back with consternation.
I had avoided mammograms because I feared the pain they caused. But once 45, I should have gotten tested. Fear, guilt, sadness caged me all those bleak years as I counted days wishing desperately to be declared a survivor.
Cancer diminished me. But when it opened a second ugly chapter in my life due to a possible case of “medical negligence,” I was dumbstruck and left floundering. Five years later when I thought I had reason to celebrate, I began to feel inexplicably drained. On 20 July, 2012, my sister rushed me breathless to hospital.
As I lay in the Intensive Care Unit, perspiration drenched my body. Dr. G, the cardiologist, diagnosed my condition as heart failure, a critical disease. She did not guarantee my survival. But I survived.
The cause of my disease remained a mystery. I did not have coronary disease which was known to cause heart failure.
A year later, I accidentally learnt that chemotherapy had damaged my heart. “Didn’t your medical oncologist advise a 2D Echocardiogram after each chemo?’” Dr. C asked while treating me for pneumonia. Dazed, I slowly shook my head. Looking at the list of my medicines, the doctor pointed at one: ‘Epirubian is notorious for causing heart failure. I wish it had been substituted.’
I felt clobbered.
How will I go through this? A second critical disease from the treatment of the first! I bit my pillow to stem my tears.
The first time my Echo had showed a drop in my ejection fraction (EF), the alarmed look on the technician’s face told me that all was not well.
I visited different doctors, including my oncologist, between 2009 and 2011 with my annual D-Echo reports. I was concerned that my EF had been dropping since 2008 by 5% every year. When the EF reached 45% in 2011, a doctor who treated heart patients, allayed my fears and said “Your EF is ‘normal’. In 2012, they were proved wrong. They had not understood my disease but I was the sufferer not a doctor. I couldn’t question their judgement.
With its ups and downs, monthly tests, checkups, depression, anxiety, repeated hospitalizations for bouts of pneumonia and congestion due to low EF, heart failure took its toll for six years. I often thought of Dr. T and wondered why she had brought me to this pass? When I asked Dr. S why my heart had not been monitored during chemo, he said, “Only Dr. T can answer that.” But Dr. T had resigned and moved out.
“Where is she now?” I asked her assistant.
“We don’t know.”
Disheartened with their replies, I walked out of the hospital wearily, telling myself, “I’ll fall very ill if I go after that woman. Let me look after my health and stay well as much as is possible.” I was weak and took slow, small steps to avoid straining my heart.
In 2018, my heart deteriorated rapidly. My heart failure reached end-stage. As a last resort, Dr. G suggested the heart transplant which I underwent to save my life.
But I had spent 5 million rupees on the high risk intervention and needed another 0.3 million yearly for immuno-suppressants, medical monitoring and monthly tests. Heart transplants make one disease-free but medicines have to be taken lifelong. My pension is not very big. I worried that 90 percent of my lifetime savings had vaporized because of a doctor’s negligence!
I wanted to take legal action. But I could not make a headway because hospital practices make it near impossible to prove a doctor’s negligence and too, eleven years had pasted after my system had been poisoned with Epirubicin! Medical records, including doctors’ notes, are preserved for a decade or so but are eventually destroyed for want of space.
The onus to prove medical negligence was on me. I was a lone patient standing against an organization.
My case was “legally weak” in every way. I accepted the reality and dropped the idea of going further. At 70, and after years of disease I did not have enough energy left to excavate the evidence that could help me win my case.
We are lay persons and do not have adequate knowledge about diseases nor about the pros and cons of their treatment. We hesitate to question our doctors lest they feel offended. The truth is it is we who need them.
After my recovery, I have come to believe that though the legal odds are stacked against patients, we must not consider ourselves helpless in guarding our health.
My experience as a transplant recipient was good because of a competent cardiac team. I have since, visited websites of hospitals undertaking heart transplants to equip myself with ways in which I can prevent the side effects. I have studied the signs to watch for and proactively consult my doctors whenever I spot variations in my reports. They too reach out because I have told them I need their continuous support. It makes me feel confident.
As for a re-look at the law, I hope someday, someone will petition and the opaque law will be revised suitably. The good tidings is that lately (2016), India’s Judicial forums have signalled an “increased need of the doctors to engage with the patients during treatment, especially when the line of treatment is contested, has serious side effects and alternative treatments exist”.
There is hope but it needs a push to make it a reality.