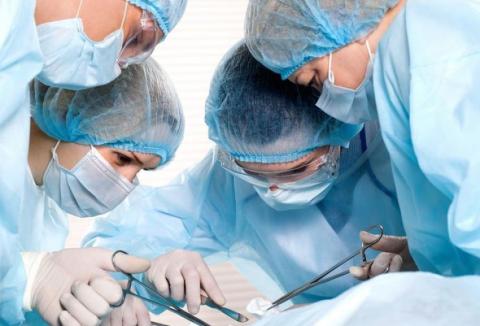
Mr Clark was 60 and remarkably well. He lived at home with his wife where they “looked after each other”. He walked his little dog twice each day. He required a nephrectomy for an aggressive renal tumour. My consultant, Dr Roberts expected a large blood loss and was prepared: additional large intravenous cannulae, a central line, arterial line, six units of blood in the fridge, blood bank on standby for more.
The surgery was painstakingly difficult as the surgeon meticulously dissected out the kidney avoiding the tumour and vessels. The kidneys work hard and receive 20% of the cardiac output, around 1.5 litres of blood per minute. 25mls per second is a lot of blood.
The surgeon freed the renal vein and applied a clamp. A suture was slung around and pulled tight. The bleeding started immediately as the suture slid and transected the wall of the vein with the ease of a cheese wire.
Another suture was requested, hurriedly mounted and passed to the surgeon. Slowly and carefully, despite continual blood spillage, noisy suckers and soaked swabs, the surgeon placed the second suture. The same thing happened and the bleeding intensified. At the head end we could see the surgeon’s distress.
“Whenever I try to suture it, it disintegrates” he said, arms raised at the perplexity of it. What do you do when the usual treatment compounds the problem?
He re-sited the clamp proximally but there were many ragged breaches in the vein wall, weakened due to infiltrating tumour.
We actioned our plan. Opening drips on both sides, clear fluid pouring into the circulation. The atmosphere had changed: a sinister quiet had settled, punctuated only with short requests to the nurses by the surgeon and Dr Roberts. We swapped our clear fluid for two bags of blood. Then another two.
“Phone the lab and ask for six more bags fast” instructed Dr Roberts
“Give us a minute to catch up,” he asked the surgeon.
The surgeon packed the bleeding area with large swabs to temporarily dam the flow while we restored the circulating volume.
The large swabs turned quickly red and were replaced. Haemostatic gauze was called for and placed over the bleeding vein. The blood continued to spill. The large vein could not contract as an artery would.
We used all six bags of blood. More was 30 minutes away.
“Get the O negative,” Dr Roberts said, “keep pushing in clear fluid, colloid, anything down those lines”.
I nodded, realising the gravity of the situation.
“How is he at your end?” the surgeon asked, hoping for reassurance. We weren’t winning either.
A nurse wiped the blood from the surgeon’s visor and put absorbant pads on the floor where blood was accumulating, the drapes long since saturated. An adrenaline syringe was now running. As its rate increased exponentially, I could feel my own adrenaline levels increase too.
The battle continued: more stitches, more swabs, more hands in Mr Clark’s abdomen, more blood, more instruments, more tension and more failure.
I took potent syringe jets of adrenaline from the resuscitation trolley and began to administer large boluses at a time. Dr Roberts noticed and nodded. The bags of fluid were squeezed in under pressure then thrown into a pile on the floor: they would be counted later. The numbers on our screen were dropping, flashing, alarming: the exsanguination relentless.
The capnograph dwindled. The one trace that confirms life was non-reassuring. Mr Clark was grey, his face waxy. The bleeding continued to outpace us and culminated in cardiac arrest. Dr Roberts commenced cardiac compressions. I knew this was futile; cardiac arrest was only a symptom of the problem. The purpose was to confirm everything had been done and allow a consensus opinion to be confirmed. It was time to stop.
The surgeon left the operating table, ripping off his gown and slamming it into the bin. The door to the scrub room banged shut. Momentary silence blanketed the theatre before we each felt the need to be purposefully engaged. I silenced the alarms and closed the drips, unsure of protocol. The surgeon’s assistant closed the abdomen. Thick, coarse sutures lacking precision or planning.
Dr Roberts turned off the anaesthetic gases and with reluctance, turned off the ventilator. I felt a morbid finality, never before experienced. It was over. The procedure, the anaesthetic, the life.
My overriding thoughts at that moment were not for Mr Clark, nor his wife. Not for the surgeon or Dr Roberts. They were for me and were mostly of relief. I was glad I was not in charge, was not required to make the big decisions nor standby the outcomes. Glad for once that I was a trainee with responsibility only to learn. No-one had done anything wrong. No vital step was forgotten yet the patient died. I was not ready to carry that weight.
It would be 14 years later that I would find myself in charge of a similar case, and would carry the outcome heavily on my shoulders. By then I would be experienced and confident in my practice, yet still, it would not sit comfortably. I doubt it ever does.